Your oral health is a vital component of your overall well-being, far beyond just maintaining a beautiful smile. Ignoring persistent dental warning signs can exacerbate pain, lead to more complex and costly treatments down the road, and even contribute to serious health conditions like cardiovascular disease, diabetic complications, and cognitive decline.
It’s encouraging to note that Canada boasts high standards in oral health, with approximately 75% of Canadians visiting a dental clinic annually, and over 80% believing they have good or excellent oral health. This proactive approach is crucial, as timely dental care can prevent minor issues from becoming major emergencies. However, even with regular check-ups, unexpected dental problems can arise, signalling an urgent need to see your dentist right away. Recognizing these dental warning signs is the first step towards safeguarding your oral and overall health. In this post, we will explore five critical indicators that demand immediate professional attention, helping you understand when it’s time to prioritize your dental health.
1. Persistent Toothache: Your Body’s Urgent Warning
A toothache is more than just an inconvenience; it’s your body sending an urgent dental warning sign that something is wrong. Pain can range from mild discomfort to severe, throbbing sensations, often intensifying at night due to increased blood flow to the head and fewer distractions. Common culprits behind persistent toothaches include deep cavities, infections reaching the tooth pulp, or trauma to the tooth. Grinding your teeth at night, a habit many people are unaware of, can also lead to significant dental pain, worn enamel, and even jaw muscle strain, headaches, and sleepiness.

Consequences of Ignoring Severe Tooth Pain
If left unaddressed, a simple cavity can penetrate deeper into the tooth’s interior, damaging the dentin and infecting the pulp or roots. This can escalate rapidly, potentially leading to an abscess—an enclosed pocket of infection that can spread to the jawbone and beyond, posing a serious health risk if left untreated.
Ignoring a toothache can have dire consequences beyond localized pain. What might initially require a simple filling could quickly progress to the need for a root canal or even tooth extraction if the nerve is affected or the tooth cracks. Losing a tooth can then trigger a cascade of new problems, including bite misalignment, shifting of adjacent teeth, and jawbone deterioration.
Temporary Relief from a Toothache
For temporary relief until you can see a dentist, you can try over-the-counter pain medication like paracetamol or ibuprofen, apply a cold compress to the affected area, or elevate your head while sleeping to reduce blood flow and pressure. Avoiding cold, acidic, or sugary foods before bed can also prevent aggravation of existing cavities. Remember, a toothache is a clear call to action from your body; seeking prompt professional help is crucial to prevent further damage and alleviate discomfort.
2. Bleeding and Swollen Gums: More Than Just a Minor Irritation
Bleeding and swollen gums are significant dental warning signs of underlying oral health issues that demand immediate attention, rather than being dismissed as mere minor irritations. These symptoms, often accompanied by redness and tenderness, are primary signs of gingivitis, an early stage of gum disease. Gingivitis is typically caused by the accumulation of plaque, a sticky film teeming with bacteria, that forms on your teeth after eating or drinking. If this plaque isn’t effectively removed through regular brushing and flossing, it hardens into tartar, which can then spread below the gum line, exacerbating inflammation and infection.
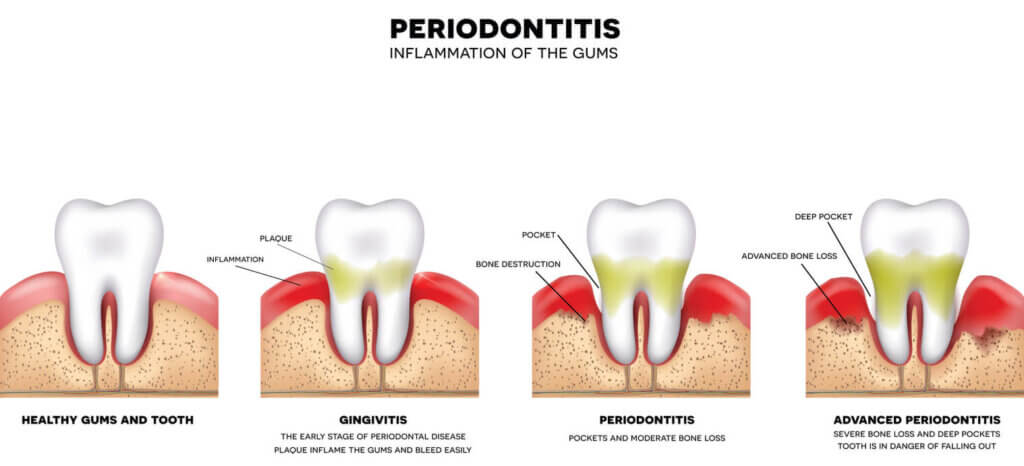
The Implications of Ignoring Gum Issues
The implications of ignoring bleeding and swollen gums extend far beyond your mouth. Untreated gingivitis can advance to periodontitis, a more severe form of gum disease where the infection begins to destroy the periodontal tissues that support your teeth, including the gums, ligaments, and jawbone. This destruction can lead to gum recession, exposure of tooth roots, and ultimately, tooth loss.
Furthermore, the harmful bacteria from gum disease can enter your bloodstream through bleeding gums, potentially leading to systemic health complications. Harvard Medical School highlights a concerning link between gum disease and a two to threefold increased risk of heart attack, stroke, and other serious cardiovascular events, often due to chronic inflammation.
Other systemic health issues linked to poor oral health and spreading bacteria include diabetic complications, respiratory problems like pneumonia, and even neurological conditions such as Alzheimer’s disease and dementia. Maintaining healthy gums through consistent brushing (at least twice a day for two minutes with fluoride toothpaste) and daily flossing is paramount in preventing plaque buildup and subsequent gum disease. Regular professional cleanings are essential to remove plaque and tartar that home care might miss, helping to keep your gums healthy and prevent these serious systemic issues.
3. Sensitivity to Hot or Cold: A Sign of Underlying Damage
Experiencing sharp, fleeting pain when consuming hot or cold foods and beverages, or even when exposed to cold air, is a common symptom of tooth sensitivity. While it might seem like a minor annoyance, persistent sensitivity is a critical indicator of underlying dental damage that warrants prompt professional evaluation. This sensitivity often occurs when the protective outer layer of your teeth, the enamel, is worn down or damaged, exposing the softer, more porous layer beneath it called dentin. The dentin contains microscopic tubules that lead to the tooth’s nerve, and when exposed, these tubules allow hot or cold stimuli to reach the nerve, causing pain.

Common Causes of Sudden Sensitivity
Several factors can contribute to enamel erosion and exposed dentin. Frequent consumption of sugary and acidic foods and drinks like citrus fruits, soda, or wine can erode tooth enamel, making your teeth more prone to sensitivity and decay. Brushing immediately after consuming acidic items can further weaken softened enamel, increasing its susceptibility to erosion.
Additionally, aggressive brushing with a hard-bristled toothbrush or conditions like teeth grinding can also wear down enamel and expose the dentin. Untreated cavities are another major cause of sensitivity, as the decay creates direct pathways to the tooth’s nerve.
Risks of Delaying Treatment for Tooth Sensitivity
If left unaddressed, what begins as simple sensitivity can progress to more severe issues, potentially requiring dental fillings, root canal therapy, or even tooth extraction if the decay becomes extensive and impacts the tooth nerve. While temporary relief can be found by avoiding trigger foods and drinks or using desensitizing toothpastes, these are not long-term solutions.
A dentist can accurately diagnose the root cause of your sensitivity through examinations and X-rays, recommending appropriate treatments such as fluoride treatments to strengthen enamel, dental sealants, or fillings to protect vulnerable areas, and advising on proper oral hygiene practices to prevent further damage. Proactive dental intervention is key to halting the progression of damage and preserving your tooth’s health.
4. Chipped, Cracked, or Loose Teeth: Beyond Cosmetic Concerns
A chipped, cracked, or loose tooth is more than just a cosmetic flaw; it’s a significant dental red flag that requires immediate attention. These injuries can result from various incidents, including accidents, trauma during sports, biting down on hard objects like ice or pens, or even chronic teeth grinding. While some damage might appear minor, it can lead to severe pain, increased sensitivity to temperature changes, and provide an opening for bacteria to enter the inner tooth structure, potentially causing infection or tooth loss. A deep crack, for instance, can compromise the integrity of the tooth, eventually leading to the need for a root canal or extraction if the pulp becomes infected.
Long-term Consequences of Ignoring Chipped, Cracked or Loose Teeth
Ignoring such injuries can lead to worsening conditions. A loose tooth, often a symptom of advanced gum disease, can indicate compromised bone support and risks falling out if not stabilized. A chipped tooth, if not repaired, can develop sharp edges that irritate the tongue and cheeks, or it can progress into a larger fracture, exposing the sensitive dentin or pulp. In cases of a knocked-out tooth, immediate action is critical: retrieving the tooth, rinsing it gently, and attempting to reinsert it or placing it in milk before rushing to the dentist can significantly increase the chances of saving it.
Protecting your teeth is paramount; wearing a mouthguard during contact sports is a simple yet effective preventative measure against such injuries. Your dentist can assess the extent of the damage and recommend the best course of treatment, ranging from dental fillings for minor chips and cracks to dental crowns for more extensive damage, or even dental implants for lost teeth. Prompt intervention not only alleviates pain and discomfort but also prevents further complications and preserves your smile’s structure and function.
5. Persistent Bad Breath or Foul Taste: Not Just a Hygiene Issue
Persistent bad breath, medically known as halitosis, or a lingering foul taste in your mouth, is often a clear indication of underlying oral health problems that extend beyond simple hygiene. While temporary bad breath can result from certain foods, chronic issues typically stem from the accumulation of plaque and bacteria in your mouth. Bacteria thrive in the mouth, especially when food particles are left behind, producing volatile sulfur compounds that cause an unpleasant odor. This can be particularly problematic if plaque is left untreated, turning into tartar, which cannot be removed by brushing alone.

Additional Factors Contributing to Bad Breath
Beyond plaque buildup, more serious conditions contribute to persistent bad breath and foul taste. Gum disease, characterized by swollen and bleeding gums, creates pockets where bacteria can proliferate, leading to chronic bad breath that is difficult to mask. Untreated tooth decay or cavities can also harbor bacteria and food debris, contributing to a foul taste and odor.
What’s more, a dry mouth, often caused by certain medications or insufficient hydration, reduces saliva production, which is crucial for washing away food particles and neutralizing acids, thereby allowing harmful bacteria to flourish and cause bad breath.
Additionally, systemic infections and certain medical conditions, even those unrelated to the mouth, can also manifest as persistent bad breath or a strange taste. Relying solely on mouthwash for a fresh feeling is a temporary fix, as mouthwash is an adjunct to, not a substitute for, proper brushing and flossing.
If these issues are ignored, the underlying conditions will worsen, leading to more extensive dental problems and potentially affecting your overall health. An unpleasant taste or odor could also be a sign of pus draining from an abscess, which is a serious infection requiring immediate attention. A comprehensive dental examination is essential to identify the root cause of persistent bad breath or a foul taste, enabling your dentist to provide targeted treatment and help you achieve fresh breath and optimal oral health.
My Dentist at Morgan Creek: Your Partner in Lifelong Oral Health
At My Dentist at Morgan Creek, we understand that maintaining optimal oral health for your entire family is a top priority, and we are dedicated to being your trusted partner in achieving that goal in South Surrey and White Rock, BC. Our clinic offers a comprehensive range of dental services designed to cater to patients of all ages, from infants establishing their first oral hygiene habits to adults seeking advanced cosmetic or restorative treatments. We believe in a “one-stop-shop” approach, simplifying your life by enabling convenient scheduling for your entire family, fostering continuity of care, and building trusting relationships that last a lifetime.
Advanced Technology and Experienced Care
Our commitment to patient comfort and well-being is our number one priority. We always strive for gentle dentistry, employing experienced and empathetic dentists who are skilled in creating positive dental experiences, particularly for our youngest patients. We utilize cutting-edge dental technology, including 3D Sirona imaging, rotary endodontic equipment, apex locators, CEREC® CAD/CAM technology for same-day crowns, 3D printing for surgical guides, and digital X-rays that minimize radiation exposure. For patients with dental anxiety, particularly fear of needles, we offer innovative solutions like The Wand Single Tooth Anaesthesia (STA) system, a computer-assisted technology that delivers anesthesia with precision, reducing discomfort and eliminating unwanted facial numbness. This focus on advanced technology and compassionate care ensures that your visits are as comfortable, efficient, and pain-free as possible.
Our comprehensive services include preventive dentistry, general dental care, pediatric dentistry, cosmetic dentistry (including teeth whitening, veneers, and Invisalign), dental implants, root canal treatments, and emergency dental care, ensuring all your family’s needs are met under one roof. We are also proud to be one of the first dental offices in the area to introduce guided implant surgery and 3D printing technology, attracting many patient referrals for complex cases.
With a strong 4.9-star rating from over 400 clients, our dedication to excellence shines through. We also offer flexible financing options and work with most insurance plans, making quality dental care accessible for everyone.
Don’t Wait: Take Action for Your Oral Health Today!
Recognizing the signs that demand immediate dental attention is the first crucial step towards safeguarding your oral and overall health. Whether you’re experiencing a persistent toothache, bleeding gums, heightened sensitivity, a chipped tooth, or lingering bad breath, these symptoms are your body’s clear signals that professional help is needed. Ignoring them can lead to escalating pain, more complicated and expensive treatments, and even serious systemic health issues. Your smile is our goal at My Dentist at Morgan Creek, and your oral health is our top priority.
Don’t let dental problems compromise your well-being or disrupt your daily life. Our caring and professional team at My Dentist at Morgan Creek in South Surrey and White Rock is ready to provide the personalized, gentle care you deserve. We offer same-day emergency appointments for urgent concerns, with extended hours and Saturday availability to accommodate your busy schedule. You and your family might also be eligible for the new government dental plan; call us or fill out our form to find out more.
Let’s work together to give you a healthy mouth and a confident smile. Contact us today to book your dental appointment.
Frequently Asked Questions (FAQs)
Q1. Can stress affect my teeth and gums?
While not explicitly detailed in the provided sources, stress is commonly linked to oral health issues. High stress levels can lead to habits like teeth grinding (bruxism), which can cause tooth pain, worn enamel, and jaw issues. Stress can also weaken the immune system, making you more susceptible to gum disease and infections. The provided sources mention links between oral bacteria and various systemic illnesses, including “stress related issues” and “depression,” which suggests a broader understanding of stress’s impact on health.
Q2. Are dental X-rays safe during pregnancy?
Yes, dental X-rays are generally considered safe during pregnancy, especially with modern digital X-ray technology. Digital X-rays use significantly less radiation than traditional ones, minimizing exposure for both the expectant mother and the baby. However, it’s always advisable to inform your dentist if you are pregnant, as they will take extra precautions, such as using lead aprons, to ensure maximum safety. Scheduling a prenatal dental checkup early in your pregnancy is recommended to discuss any concerns and create a personalized oral hygiene plan.
Q3. What are the differences between a dental filling and a crown?
A dental filling is used to repair a tooth affected by decay, cracks, or fractures by removing the damaged portion and filling the space with materials like composite resin or amalgam. Fillings are typically used for smaller areas of damage. A dental crown, on the other hand, is a cap that covers and protects a significantly damaged or discoloured tooth, restoring its shape, function, and appearance. Crowns are used when a tooth has more extensive damage or after procedures like a root canal to protect the treated tooth. My Dentist at Morgan Creek offers both, including CEREC® 1 Appointment Crowns for quick restorations.
Q4. Can I whiten my teeth if I have sensitive teeth?
Yes, having sensitive teeth does not necessarily mean you cannot whiten them. Professional dental practices offer options to help reduce sensitivity during treatment, ensuring a more comfortable experience. It’s crucial to consult with your dentist before starting any whitening treatment, especially if you have sensitive teeth, as certain conditions like tooth decay or gum infection might preclude you from undergoing teeth whitening initially. Your dentist can assess your specific needs and recommend the safest and most effective whitening method, such as professional in-office treatments or customized at-home kits with appropriate guidance.
Q5. What should I do if I have severe tooth pain at night?
For severe nighttime tooth pain, take over-the-counter pain medication as directed on the package, apply a cold compress to the outside of your face for 15-20 minutes at a time, and sleep with your head elevated. Avoid placing aspirin directly on the tooth or gums, as this can cause tissue damage. Contact your dentist first thing in the morning, or visit an emergency room if you develop fever, facial swelling, or difficulty swallowing.





